Compliance is often discussed as a hurdle to overcome or a set of boxes to tick before an inspection. In reality, for those managing nursing homes, children’s residentials, and supported living services, compliance is the quiet heartbeat of a safe operation. It is the framework that allows high-quality care to happen consistently. As a provider of CQC-regulated support packages this has been brought even closer to home at S.N.G. Delivering care across individual packages (often in fast-moving, real-world settings) means the standard must travel with the work: the right people, the right plan, the right documentation, and the right oversight, every day.
For a manager in the UK health and social care sector, the weight of regulation can feel heavy. However, when we strip away the jargon, compliance is simply the process of proving that we do what we say we do. It is about ensuring that every person under our care is safe, treated with dignity, and supported by a team that is fit for purpose.
The Shift to the Single Assessment Framework
The introduction of the CQC (Care Quality Commission) Single Assessment Framework in July 2022 changed the mechanics of oversight. The regulator moved away from the old system of intensive, one-off inspections toward a model of continuous monitoring. This means that compliance is no longer something you “cram” for once every few years. It is an ongoing conversation between the provider and the regulator.
This new approach relies heavily on “Quality Statements.” These statements replace the old Key Lines of Enquiry (KLOEs) and focus on specific outcomes for the people using the service. For managers, this means the evidence you collect must be live and dynamic. It is no longer enough to have a dusty policy folder on a shelf. You must be able to show, through real-time data and feedback, that those policies are active in the daily lives of your residents and staff.
The Five Pillars of Quality
The CQC continues to evaluate every service against five key questions. These pillars provide a clear structure for any compliance strategy.
Safety is the first priority. This involves more than just avoiding accidents. It is about robust safeguarding, meticulous medication management, and infection control. It also means having a staffing model that is resilient. At SNG Healthcare, we understand that a safe service is one where risks are identified early and mitigated with common sense and care.
Effectiveness looks at the outcomes of the care provided. Are the people you support reaching their goals? Is the care based on the latest best practices? This requires a commitment to staff training and a culture where learning is encouraged. When staff have the right skills, they feel confident, and that confidence translates into better care.
Caring is the most human element of compliance. It measures whether staff treat people with kindness and respect. While it can feel difficult to “measure” compassion, the CQC looks for evidence of person-centred care. This means involving individuals in their own care decisions and respecting their privacy and choices at all times.
Responsiveness is about how a service adapts to changing needs. A compliant service is one that listens. Whether it is responding to a formal complaint or adjusting a support plan because a person’s health has changed, being responsive shows that the individual is at the centre of the service.
Well-led is perhaps the most critical pillar for managers. It evaluates the governance and leadership of the service. A well-led service has clear lines of accountability and a culture of transparency. It is about having the humility to admit when things go wrong and the resolve to fix them.
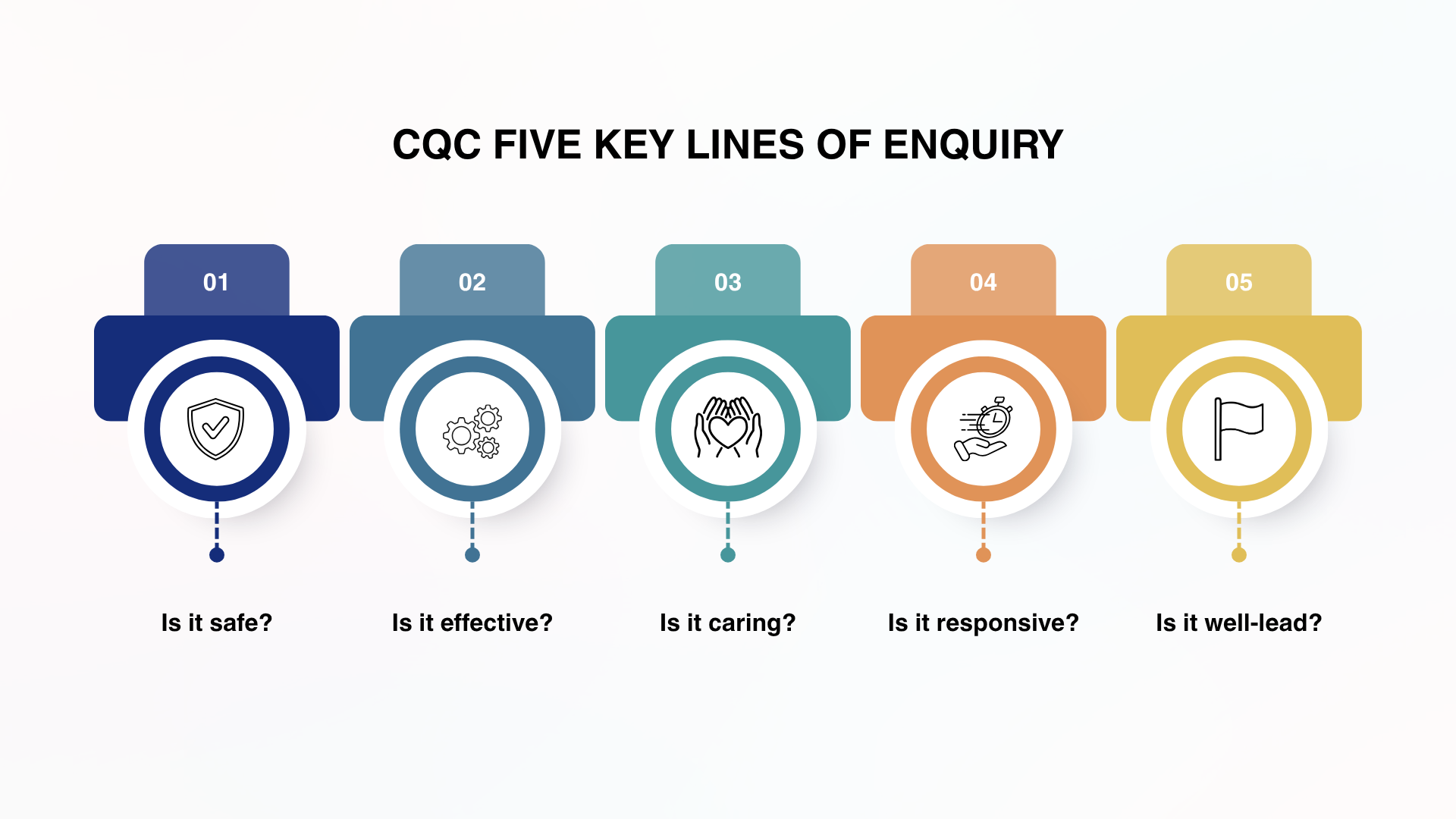
CQC Five Key Lines of Enquiry
The 16 Fundamental Standards of Care as a Baseline
Beneath the high-level assessments sit the 16 Fundamental Standards. These are the legal requirements that every registered provider must meet by law. They represent the floor below which care must never fall. They include:
- Person-centred care: Tailoring treatment to the individual.
- Dignity and respect: Ensuring privacy and equality.
- Consent: Always seeking permission before care is given.
- Safety: Providing care in a safe way with qualified staff.
- Safeguarding from abuse: Protecting people from any form of harm.
- Food and drink: Meeting nutritional and hydration needs.
- Premises and equipment: Ensuring the environment is clean and secure.
- Complaints: Having a transparent system to listen and act.
- Good governance: Having systems to check the quality and safety of care.
- Staffing: Employing “fit and proper” persons who are supported and trained.
- Duty of Candour: Being open and honest when things go wrong.
For a manager, these standards are the checklist for integrity. Meeting these 16 points ensures a service is built on a foundation of rights and safety.
The Importance of Robust Documentation
In the eyes of a regulator, if an action is not documented, it did not happen. This is often where well-meaning services struggle. Gaps in care notes or inconsistent records can make a high-quality service look disorganized or unsafe.
Moving toward digital care records is one of the most effective ways to maintain compliance. Digital systems provide a clear, time-stamped audit trail. They allow managers to see at a glance if a medication has been missed or if a care plan is overdue for a review. This level of oversight is essential for maintaining the “Well-led” rating. It allows you to move from being reactive to being proactive, identifying trends before they become problems.
Staffing and the “Fit and Proper Person” Requirement
A significant part of compliance involves the people you employ. Regulation 19 focuses on ensuring that all staff are “fit and proper” for their roles. This involves rigorous background checks, including DBS clearances and verified references.
However, compliance in staffing goes beyond the initial hire. It includes ongoing supervision, appraisals, and professional development. A compliant service ensures that its team is not just qualified on paper, but supported in practice. When staff feel valued and have a clear understanding of their responsibilities, they are much more likely to uphold the standards of the organization.
Managing Complaints and Feedback
Regulation 16 requires every provider to have a clear and accessible complaints procedure. A healthy compliance culture views complaints not as a threat, but as vital intelligence.
An effective complaints process should be easy for anyone to use. It should ensure that concerns are acknowledged quickly and investigated thoroughly. Most importantly, the findings should be used to drive improvement. When a manager can show a CQC inspector how a specific complaint led to a change in policy or practice, it provides powerful evidence of a “Well-led” and “Responsive” service.
Final Thoughts on a Compliance Mindset
Compliance is the foundation upon which great care is built. It provides the safety and structure that allow care professionals to do their best work. For SNG Healthcare, being a CQC-registered provider means we hold ourselves to these high standards every day.
By treating compliance as a continuous discipline rather than a periodic event, managers can create services that are not only safe and effective but also resilient and transparent. It is about leading with insight and ensuring that every decision is made with the well-being of the individual in mind.
Please don’t hesitate to contact us to discuss anything that was mentioned here or if you are looking for high-quality, CQC-regulated support for your loved ones or your service. We’re here for a friendly, no-pressure chat whenever you need us.